Cervical radiculopathy arises from cervical nerve root compression, causing upper extremity pain and deficits; effective management involves physical therapy, medication, and manual techniques.
Defining Cervical Radiculopathy
Cervical radiculopathy is a specific condition characterized by the compression or irritation of one or more nerve roots in the cervical spine. This compression disrupts the normal function of the nerve, leading to a constellation of symptoms radiating from the neck into the shoulder, arm, and hand. The root cause often stems from degenerative changes within the vertebral structures, such as disc herniation or spinal stenosis, directly impacting the nerve root.
Consequently, individuals experience pain, sensory alterations – including numbness or tingling – and potential motor weakness in the affected dermatome. Accurate diagnosis, often aided by imaging like MRI, is crucial for developing an effective physical therapy protocol focused on pain management and functional restoration.
Prevalence and Impact
Cervical radiculopathy represents a common musculoskeletal condition, significantly impacting quality of life and functional capacity. While precise prevalence figures vary, it’s a frequent reason for seeking medical attention, particularly among middle-aged adults experiencing neck and arm pain. The condition’s impact extends beyond physical discomfort, often leading to lost workdays, reduced participation in daily activities, and psychological distress.
Effective management, including a well-structured physical therapy protocol, is vital to minimize long-term disability. Early intervention can prevent chronic pain and restore optimal neck and upper extremity function, improving overall well-being and productivity.
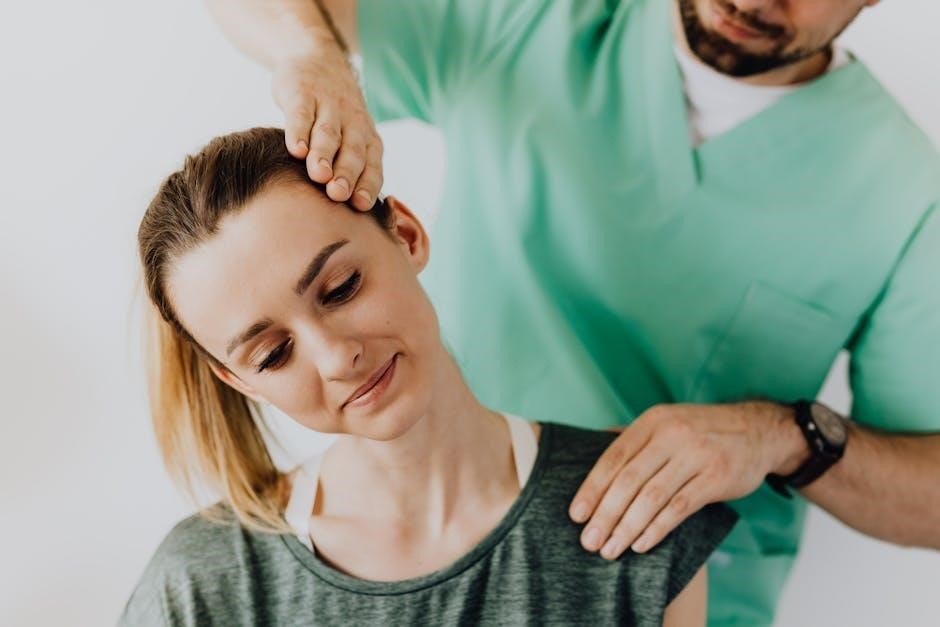
Etiology and Pathophysiology
Degenerative changes within the cervical spine, leading to nerve root compression, are the primary cause of cervical radiculopathy and subsequent symptoms.
Degenerative Changes in Vertebral Structures
Degenerative alterations within the cervical spine represent a core etiological factor in cervical radiculopathy. These changes encompass several processes, including osteoarthritis, disc degeneration, and the formation of bone spurs (osteophytes). Over time, the intervertebral discs lose hydration and elasticity, diminishing their ability to cushion the vertebrae. This leads to narrowing of the spinal canal – spinal stenosis – and the foraminal openings through which nerve roots exit.
Consequently, these structural modifications contribute to nerve root compression or irritation. The gradual nature of these degenerative processes often means symptoms develop insidiously, although acute exacerbations can occur. Understanding these structural changes is crucial for developing targeted physical therapy interventions aimed at mitigating compression and restoring optimal spinal mechanics.
Nerve Root Compression Mechanisms
Nerve root compression in cervical radiculopathy occurs through several interconnected mechanisms. Direct mechanical compression from osteophytes, disc herniations, or thickened ligamentum flavum are primary contributors. However, inflammation surrounding the nerve root, often due to degenerative changes, also plays a significant role, increasing sensitivity and contributing to symptoms.
Foraminal stenosis, the narrowing of the bony opening where nerve roots exit, further exacerbates compression. These compressive forces disrupt nerve root physiology, leading to impaired nerve conduction and the characteristic pain, sensory changes, and weakness observed in radiculopathy. Physical therapy aims to address these mechanisms by reducing inflammation, restoring space, and improving nerve mobility.

Clinical Presentation & Diagnosis
Diagnosis relies on correlating clinical findings – pain radiation, sensory deficits, and weakness – with imaging like MRI or CT scans to pinpoint nerve root compression.
Pain Characteristics (Location, Radiation, Quality)
Pain associated with cervical radiculopathy typically originates in the neck, often radiating into the shoulder, and down the arm following a specific dermatomal pattern. Patients frequently describe the pain as sharp, burning, or aching. The location of the pain helps identify the affected nerve root; for example, C5 radiculopathy often presents with lateral shoulder pain, while C7 radiculopathy commonly causes pain in the triceps region.
Pain can be exacerbated by certain neck movements, such as extension, flexion, or rotation. Some individuals experience paresthesias (tingling or numbness) alongside the pain. The quality of pain can vary, ranging from a constant, dull ache to intermittent, shooting pains. Accurate pain characterization is crucial for diagnosis and guiding treatment strategies within a physical therapy protocol.
Sensory Deficits & Weakness
Sensory deficits in cervical radiculopathy often manifest as numbness, tingling, or diminished sensation in the upper extremity, corresponding to the affected dermatome. Light touch, pinprick, and proprioception may be impaired. Weakness typically affects specific muscle groups innervated by the compromised nerve root. For instance, C5 radiculopathy can cause weakness in shoulder abduction and external rotation.
C6 radiculopathy frequently presents with wrist extensors weakness, while C7 impacts triceps strength. Assessing these neurological signs is vital during a physical therapy evaluation. The degree of sensory loss and weakness helps determine the severity of nerve root compression and guides the development of a targeted rehabilitation protocol.
Diagnostic Imaging (MRI, CT Scan)
Diagnostic imaging plays a crucial role in confirming cervical radiculopathy and identifying the underlying cause. MRI (Magnetic Resonance Imaging) is generally the preferred modality, providing detailed visualization of soft tissues like the spinal cord and nerve roots, revealing compression or inflammation. CT (Computed Tomography) scans are useful for assessing bony structures, identifying vertebral fractures, or significant degenerative changes.
While imaging aids diagnosis, clinical correlation is essential. A physical therapy protocol is often initiated based on clinical findings, even before imaging results are available, focusing on symptom management and functional restoration. Imaging helps rule out other conditions and guides long-term treatment planning.

Physical Therapy Assessment
Comprehensive assessment includes postural analysis, range of motion evaluation, neurological testing for sensory deficits and weakness, and pain provocation tests to guide treatment.
Postural Assessment
A thorough postural assessment is crucial, observing static and dynamic postures. Forward head posture, rounded shoulders, and thoracic kyphosis are commonly observed in individuals with cervical radiculopathy, contributing to nerve root compression. The therapist will evaluate head position relative to the shoulders, shoulder height symmetry, and spinal curves.
Assessment includes observing the patient in standing, sitting, and functional movements. Muscle imbalances, such as tight pectoral muscles and weak scapular stabilizers, are identified. This evaluation informs the development of a targeted exercise program to restore optimal alignment and reduce stress on the cervical spine, ultimately alleviating nerve root irritation and improving function.
Range of Motion Evaluation
Assessing cervical range of motion (ROM) is essential to identify limitations impacting function. Active, passive, and resisted ROM are evaluated for flexion, extension, lateral flexion, and rotation. Pain provocation during specific movements helps pinpoint the affected nerve root. Decreased ROM often indicates muscle guarding, inflammation, or joint restrictions.
The therapist notes any compensatory movements during testing. Measurements are documented using a goniometer for objective tracking of progress. ROM deficits guide the selection of appropriate mobilization techniques and stretching exercises to restore normal joint mechanics and reduce nerve root compression, facilitating improved movement patterns.
Neurological Examination
A thorough neurological exam assesses sensory and motor function to identify the specific nerve root involved. This includes testing myotomes – muscle groups innervated by specific nerve roots – for weakness. Dermatomes, areas of skin supplied by each nerve root, are tested for altered sensation like numbness or tingling.
Deep tendon reflexes (biceps, triceps, brachioradialis) are evaluated for asymmetry or diminished responses. Spurling’s test, involving cervical compression, can reproduce radicular pain. The exam helps differentiate cervical radiculopathy from other conditions and guides targeted treatment strategies to address neurological deficits and improve nerve function.
Physical Therapy Goals
Primary goals include diminishing pain, restoring optimal cervical and shoulder function, and enabling return to activities through targeted exercises and education.
Pain Reduction
Initial pain management focuses on decreasing nociceptive input and modulating pain perception. This involves utilizing modalities like heat, ice, or transcutaneous electrical nerve stimulation (TENS) to alleviate muscle spasm and inflammation. Gentle, pain-free range of motion exercises are introduced to prevent stiffness without exacerbating symptoms.
Pharmacological interventions, such as non-steroidal anti-inflammatory drugs (NSAIDs) or gabapentin, may be used adjunctively, as indicated by a physician. Patient education regarding activity modification and proper posture is crucial to avoid aggravating factors. The aim is to establish a baseline of pain control, preparing the patient for more active rehabilitation phases.
Functional Restoration
The ultimate goal is to restore the patient’s ability to perform daily activities without pain or limitations. This phase incorporates advanced strengthening and endurance exercises targeting the cervical, scapular, and shoulder musculature; Proprioceptive training enhances neuromuscular control and stability, crucial for preventing re-injury.
Functional retraining involves simulating work or recreational tasks, gradually increasing complexity and load. A comprehensive home exercise program is essential for maintaining gains. Addressing psychosocial factors, like fear-avoidance beliefs, is also vital. The focus shifts from symptom management to regaining optimal function and participation in meaningful activities.

Acute Phase Physical Therapy (0-4 Weeks)
Initial treatment focuses on pain management using modalities, gentle motion, and postural education to reduce irritation and establish a foundation.
Pain Management Techniques (Modalities)
During the acute phase, pain management is paramount. Utilizing modalities like cervical traction can help decompress nerve roots and alleviate discomfort. Furthermore, the application of heat or cold therapy – depending on patient preference and response – can effectively reduce muscle spasm and inflammation.
Transcutaneous Electrical Nerve Stimulation (TENS) is also a valuable tool, providing pain relief by modulating nerve signals. Short-wave diathermy may be considered to promote deeper tissue heating and reduce muscle guarding. Pharmacological interventions, such as non-steroidal anti-inflammatory drugs (NSAIDs) or gabapentin, as noted in current guidelines, may be used in conjunction with physical therapy to optimize pain control and facilitate early participation in rehabilitation exercises.
Gentle Range of Motion Exercises
Early in the acute phase, gentle range of motion (ROM) exercises are crucial to prevent stiffness and maintain joint mobility without exacerbating symptoms. These should be performed within a pain-free range, focusing on slow, controlled movements.
Examples include chin tucks, gentle cervical retraction, and side bending. Active assisted range of motion, where the therapist supports the movement, can be beneficial if the patient has limited strength or significant pain. Avoid forceful movements or end-range stretching initially. The goal is to restore pain-free movement and prepare the cervical spine for more advanced exercises as symptoms subside, promoting early functional recovery.
Postural Education
A key component of early management involves comprehensive postural education. Patients with cervical radiculopathy often exhibit forward head posture and rounded shoulders, contributing to nerve root compression. Education focuses on recognizing and correcting these faulty patterns during daily activities.
Strategies include ergonomic advice for workstation setup, proper sleeping positions, and awareness of posture during prolonged sitting or standing. Patients are taught how to maintain a neutral spine and engage core muscles for support. Visual aids and home exercise programs reinforce correct posture. Improving postural awareness reduces stress on the cervical spine and promotes long-term symptom management.

Subacute Phase Physical Therapy (4-8 Weeks)
This phase emphasizes restoring function through targeted exercises, including cervical strengthening, nerve mobilization, and gentle manual therapy to address impairments.
Cervical Strengthening Exercises
Strengthening the cervical musculature is crucial during the subacute phase to enhance stability and support the spine, reducing nerve root compression. Exercises should begin with isometric contractions, progressing to gentle range of motion with resistance.
Examples include chin tucks, scapular retractions, and lateral neck flexions against manual resistance or using resistance bands. Focus is placed on deep neck flexor endurance, improving postural control;
Progressive overload is key, gradually increasing resistance and repetitions as tolerated. Proper form is paramount to avoid exacerbating symptoms or creating compensatory patterns. These exercises aim to restore optimal biomechanics and prevent recurrence of radiculopathy.
Nerve Mobilization Techniques
Nerve mobilization, also known as neurodynamic exercises, aims to restore optimal nerve gliding mechanics, addressing restrictions contributing to cervical radiculopathy. These techniques gently move the nervous system through its entire pathway, reducing adhesions and improving nerve conduction.
Common techniques include cervical nerve glides, upper limb tension tests (ULTTs) modified for symptom provocation, and combined movements. Precise positioning and slow, controlled movements are essential to avoid exacerbating pain.
Patient education regarding proper technique and symptom monitoring is vital. Nerve mobilization should be integrated with other interventions, like strengthening and postural correction, for comprehensive treatment.
Manual Therapy (Gentle Mobilizations)
Gentle mobilizations, a core component of subacute phase therapy, aim to restore joint mechanics and reduce nerve root irritation in cervical radiculopathy. These techniques focus on improving spinal movement and decreasing muscle guarding without causing significant pain.
Therapists employ techniques like transverse joint mobilization, gentle posterior-anterior glides, and muscle energy techniques. The goal is to address vertebral dysfunction and restore optimal joint spacing, indirectly reducing nerve compression.
Careful assessment and patient feedback guide treatment intensity. Mobilizations are combined with other interventions, ensuring a holistic approach to pain management and functional restoration.

Chronic Phase Physical Therapy (8+ Weeks)
Long-term management focuses on advanced strengthening, proprioceptive training, and functional retraining to optimize movement patterns and prevent recurrence of symptoms.
Advanced Strengthening & Endurance Exercises
Progressive resistance training is crucial during the chronic phase, building upon earlier gains. Exercises target cervical, scapular, and shoulder musculature, enhancing stability and function. Examples include weighted chin tucks, rows with resistance bands, and shoulder press variations.
Endurance work is equally important, improving the muscles’ ability to sustain activity. High-repetition, low-load exercises are favored. Isometric holds, such as maintaining a specific shoulder blade position, are beneficial. The goal is to increase stamina and reduce fatigue, allowing for prolonged participation in daily activities without symptom exacerbation. Careful monitoring of pain levels is essential throughout this progression.
Proprioceptive Training
Restoring proprioception – the body’s awareness of its position in space – is vital for long-term stability and preventing re-injury. Exercises challenge the neuromuscular system, improving joint position sense and coordination. Examples include weight shifting with eyes closed, dynamic balance activities on unstable surfaces (foam pads), and reaching tasks with perturbations.
Joint position error (JPE) can be assessed and addressed. Activities should gradually increase in difficulty, progressing from simple to complex movements. This training enhances the ability to automatically react to changes in posture and movement, protecting the cervical spine and reducing the risk of future episodes of radiculopathy.
Functional Retraining
Functional retraining bridges the gap between the clinic and real-life activities. This phase focuses on simulating tasks required for work, hobbies, and daily living, gradually increasing complexity and demand. Exercises might include lifting, carrying, reaching, and repetitive movements specific to the patient’s needs.
Proper body mechanics are emphasized throughout, ensuring efficient and safe movement patterns. The goal is to restore the ability to perform these activities without exacerbating symptoms. A progressive return to activity is crucial, monitoring for pain or neurological changes, and modifying the program accordingly to achieve lasting functional improvements.
